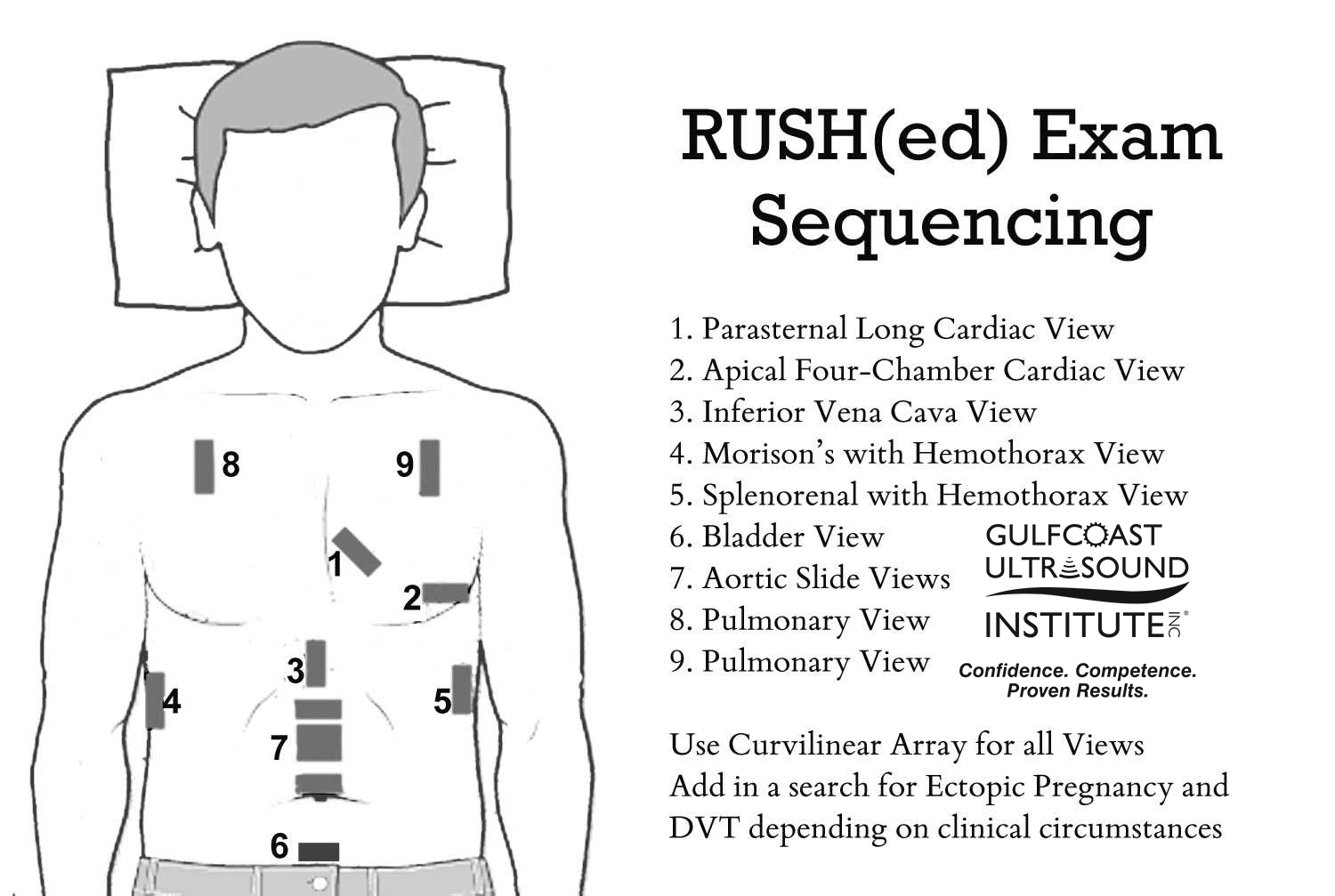
The RUSH exam provides a framework for a rapid and systematic evaluation of the non-traumatic patient in the emergency department presenting with undifferentiated hypotension. Diagnostic procedures and treatment have to be performed simultaneously for these critical patients. Point of care ultrasound allows emergency clinicians to evaluate these patients quickly at the bedside. The RUSH protocol evaluates three categories: the pump, the tank, and the pipes. Generally, the RUSH protocol begins with a cardiac evaluation, but the clinician’s judgement and clinical context should guide the progression of the evaluation.
The Pump
Ultrasound is extremely useful in determining the presence of fluid surrounding the heart. It is important to note that a pericardial effusion will appear as anechoic fluid that is anterior to the descending thoracic aorta in parasternal long axis view as opposed to pleural effusion which will appear posterior to the descending thoracic aorta.
LV contractility is evaluated and described as normal, hyperdynamic, or moderately or severely decreased. Visual assessment is generally accurate, but E point Septal Separation or calculating fractional shortening may allow a more objective assessment.
The Tank: Volume Status
The IVC is evaluated in a subxyphoid view and is measured immediately superior to the insertion of the hepatic veins. A diameter of < 2cm with >50% collapse correlates with CVP <5mmHg and suggests fluid responsiveness. A diameter > 2cm with <50% collapse correlates with CVP >10mmHg and supports the argument that the patient is not going to benefit from fluid.
It is also important to evaluate the lung windows and perform the FAST exam to evaluate for free-fluid. The presence of free fluid in the peritoneal compartment in a non-traumatic setting may suggest ruptured AAA, ectopic pregnancy or a ruptured hemorrhagic cyst. In evaluating the lung windows, the presence of multiple B-lines (vertical reverberation artifact extending from the pleural line to the far field) is suggestive of pulmonary edema. Patients will poor LV contractility, multiple B lines and a plethoric IVC are typically in cardiogenic shock. Lack of lung sliding when evaluating these windows is suggestive of pneumothorax.
The Pipes
The abdominal aorta is evaluated to determine if a hypotensive patient is presenting with a ruptured aorta. Evaluation of the abdominal aorta begins at the epigastrium and extends distally to the bifurcation of the iliac arteries. Measurement is done from outer wall to outer wall and is abnormal if > 3cm.
The thoracic aorta can be evaluated on a parasternal long axis view during the cardiac evaluation to detect a possible aortic dissection. The presence of an intimal flap may be seen if the aortic root is dissecting.
The final step of the evaluation of the pipes is to determine the presence of DVT. The lower extremities are assessed with a linear probe and compression of the common femoral, femoral, and popliteal veins is performed. A non-compressible vessel suggests the presence of a DVT. In the acute phase, the thrombus may appear hypoechoic or anechoic. Doppler evaluation to assess spontaneity and phasicity is also helpful.
Point of care ultrasound is improving diagnostic timeliness and accuracy when it matters most. Gulfcoast Ultrasound recognizes the critical role of point of care ultrasound and offers comprehensive training courses and resources taught by the leading experts in emergency and critical care medicine. Our Live and Blended courses are the perfect blend of didactic education and hands-on scanning practice that ensure you will be able to confidently and competently utilize point of care ultrasound in your clinical practice immediately. With a 3:1 instructor to participant ratio, lowest in the industry, you will have plenty of opportunity to hone your skills during your hands-on scanning sessions. Join us for one of our upcoming courses!
(727)363-4500
|
CREATE ACCOUNT
|
LOG IN
|
CART
|
Item(s) added to cart
Proceed to Checkout
Continue Shopping